
As many people (but let’s face it, not all) are aware, the NICE target for Hba1C level is 6.5% as this is the point at which relative complication risk approaches 1x the non-D population, according to the DCCT study.
We also know that the percentage of T1 people in the UK achieving this target is 8.4%, which is a staggeringly low number, and implies that many will suffer complications to some level. Below 7.5%, we achieved 29.2%, which is still a low number. Both of these are improvements on previous years.
There are many cases of hand wringing and wondering why we do “so badly” at these things, and I postulate that one of those is the continued policy that CGM is not cost beneficial in the majority of cases, and that “good control” can be achieved by the use of Self Monitoring of Blood Glucose (SMBG) or “finger pricking” alone.
Having spent the last few days relegated to the realms of this approach as a result of a CGM transmitter failure, it has hammered three things home to me.
- Achieving low Hba1C results with limited variation and few hypos is not easy using SMBG and MDI.
- The life benefits of CGM (and then automated insulin delivery systems on top of that) cannot be easily described in clinical measures.
- As T1Ds, we need to know our basics.
Whilst I realise that SMBG is far more than many have worldwide, it’s the current standard in the part of the world in which I live and the most basic of the tools we have available, so with that in mind, let’s take each of these items individually and pull them apart.
Achieving low Hba1C results with limited variation and few hypos is not easy using SMBG and MDI
I’ve mentioned before that SMBG can only ever be a point in time static measure of blood glucose data. Other than telling you whether you are high, low or in range, it cannot tell you anything else. Whilst, if you don’t check anything, it’s better than nothing, unless you “stack” tests within fifteen minutes of one another, it doesn’t tell you anything about direction or velocity of travel, and that’s as important in many decisions as simply knowing a number.
Take the below image. 12 hours on SMBG. Now within this I’m operating in a manner informed by my use of technology. I know what to expect from the insulin doses and food and how best to implement a strategy to handle it. When to wait, when to act. I’m testing regularly though, so that I can see at least some semblance of a picture and decide what to do. More importantly, I’m basing decisions on when to test more frequently on what I know I’ve done, and what the probability of the effect of that action is.
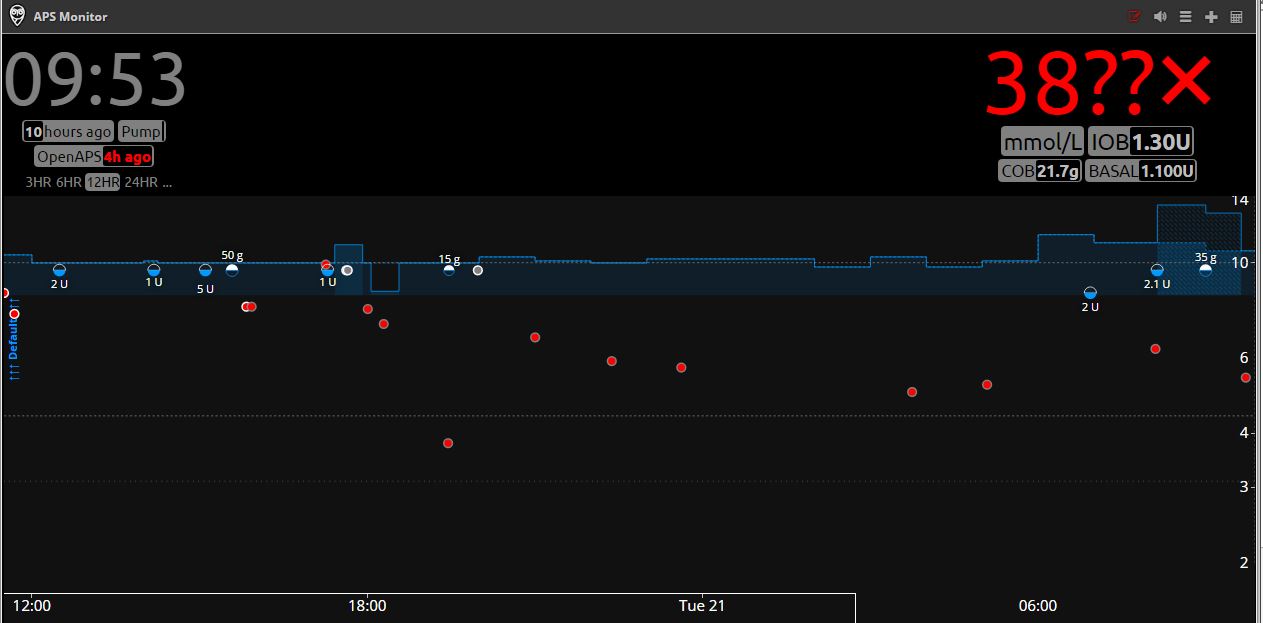
In short, I am making a ton of decisions, mostly statistical and mathematical, in order to determine if I think I’ll be okay and what I might need to do, and then interpolating the graph data to add colour to my decisions. If that seems like a lot, it is. But it’s something that I have to do if I want to maintain myself at a decent level (i.e. trying to keep variation and average levels relatively lower). If I hadn’t had technology to help me determine what the right decisions are, I’d have had to do an inordinate amount of testing to understand what my glucose profiles are. But then, I want that information to better determine what I’m doing.
Now before anyone shoots me down and says “Well you’re not expected to do SMBG without some form of education”, let me elaborate on that a little. Dose Adjustment for Normal Eating (DAfNE), a terrible name if ever there was one (the name in itself doesn’t encourage sensible eating), but a good education course for those who have not been properly introduced into how to manage on MDI and a basal bolus regime. And let’s face it, access to DAfNE is still an issue, whether that’s systemic or down to the consumer.
DAfNE doesn’t (historically at least) say, “By the way, eating high carb meals without a long pre-bolus (30 mins or more) is going to cause you to spike massively between meals” and never used to recommend two hour post meal testing to see just how that spike was. It was always “Test before meals and before bed to adjust your bolus insulin appropriately”, maybe check four hours after a meal to confirm that you have your ratios right, but it works on the assumption that you should eat the eatwell plate and pre-bolus by about 15 minutes up to pre-meal. You have to look at the target of the course and realise it is intended to make life easier for a wide range of people, many of whom don’t have strongly numerical backgrounds, which, unfortunately with all types of Diabetes, is a distinct disadvantage.
But in doing so, the advice it gives makes achieving the UK target Hba1C levels very hard. If you don’t know that eating a meal based on the eatwell plate is likely to spike you to 10+ with a bolus 10 minutes before food, and that the drop off from the meal leaves a large area under the curve pushing your average glucose up as the insulin just doesn’t act that fast, you’re never going to do anything about it. But given the nature of the help being provided, it’s better than nothing, and empirically has demonstrated a reduction in Hba1C.
If you add in alongside this the relatively blunt tool that is MDI, the ability to manage the myriad of variations that arise in dealing with glucose levels presents an even more difficult picture. You have limited ability to manage response to background glucose production, and dependent on delivery mechanism, limited ability to fine tune dosing. All in all, this presents a notable challenge.
60% of T1D Hba1C levels being greater than 7.5% paints this in a stark light. Yes living with T1D is tough, and a burden. Yes, DAfNE can be life changing and make a huge difference. No, DAfNE with SMBG is not going to bring 90% of the T1D population to an Hba1C level below 6.5% without many, and probably, severe hypos, and the resultant roller coaster. But we’ll never really know because none of the tests done as standard in the UK capture any of this stuff.
It is my hypothesis that in order to maintain low variation and low Hba1C in T1D using only SMBG and education, you need to reduce carb content of what you eat if you are eating a mixed diet. Given my own experiments across a range of technologies, I have yet to find a carb, that, eaten in even a reasonable volume, can be tamed by exogenous insulin (other than Afrezza, but that’s a different thing altogether), without some extreme pre-bolusing and a lot of shenanigans.
So for T1D management using solely SMBG and MDI techniques, alongside the carb counting of DAfNE, and other timing techniques I still think that you have to educate about reducing the volume of carbs you eat, and really, refined carbs need avoiding. Even Consultants have mentioned that the people they see in clinic with the better numbers have reduced their carb consumption. Analogue insulins are not that fast (yet).
For many people, another aspect of maintaining low levels, is a relatively consistent and limited variability diet. Knowing what’s going to happen. If you regularly change what you eat, you have to learn how it affects you, and that brings you full circle on a lot of regular testing and understanding the spikes.
The question is what are we encouraging? Are we saying you can eat anything you want to as long as you take enough insulin (as many interpret it) or are we saying that we should think carefully about what we eat as the results may not be what we want if we don’t, and providing enough information to address this? It feels as though SMBG is using a cup to put out a fire sometimes in this context. Yes it’s better than what we had before (peeing into test tubes) but it is by no means a thorough and complete view.
So while SMBG (10+ times daily to get anywhere near a decent handle on it) is a way of measuring, it’s not a way of directing. And it puts a huge amount of weight on the user’s shoulders to interpret the data and make sense of it. Or ignore it. Neither SMBG and MDI, nor with DAfNE will make the UK targets achievable by most.
The life benefits of CGM (and then automated insulin delivery systems on top of that) cannot be easily described in clinical measures
As I outlined in the previous section, in order to manage my glucose levels to ensure that I get the levels that I want (and note that it’s my decision to try and remain within the 6% Hba1C level while off all automated systems, just to see how easy it is….), I have to do a lot of decision making, and a lot of data interpretation. Even the bolus wizards that are provided on pumps and meters are relatively basic and only take account of IOB from bolusing. In short, as was a major topic at ATTD 2017, there is a significant need for decision support tools that help.
Whilst CGM alone is not fully a decision support tool, it takes away some of the steps that I outlined above when looking at finger prick data. You no longer need to interpolate data and determine where you think a glucose reading is going, trying to estimate when you’ll go low or high. That’s presented to you. In full colour if you want! You’ve now gained trajectory and velocity on your glucose data. You not only know at a point in time what the number is, but in which direction it is heading and how fast.
It’s like moving from a map to a sat nav.
With the added bonus of alerting for when you are going up too fast, going down too fast, or approaching low or high levels, it’s now possible to take your eye off your diabetes, without ignoring it, knowing that you have safety harness that you can use. In short, it relieves burden and in this case, anxiety.
It also reveals things you never knew, unless you tested far more frequently than DAfNE suggests. You can learn about post-prandial spikes, about insulin timing, and about how to deal with all these things. But to do this well, you will probably also need some form of education. And it may result in a change in how you manage your diabetes, along the lines of “Sugar Surfing“. Dynamic Diabetes Management. It works and it works well, and to achieve an Hba1C below 6.5% and low variation, it does a fantastic job.
But it also shows how difficult it is to achieve this with purely static, or pseudo dynamic data from SMBG.
And of course automated delivery systems make this even easier, relieving even more of the burden or pressure of having to make decisions on a regular basis in order to stay alive in a healthy way. That’s the non-clinical benefit. Properly used, and with the ability to disable alarms when necessary, continuous data and automated systems can reduce the amount of time spent thinking about this disease. For those who remember, it’s the difference between having a choke and an automated engine management system. There’s a whole lot less guessing required to start the car.
Now we know that this doesn’t work for everyone, and there are plenty of people that have struggled with CGM, but I wonder how the percentages break out, if you compare the proportion that struggle with CGM to the proportion that struggle with SMBG? And what education it would take to improve those metrics? All questions that I find it hard to find evidence for.
As T1Ds, we need to know our basics
As I mentioned at the start, my CGM transmitter died. 70 days ahead of the date it was supposed to. It was somewhat unexpected and rather left me in the lurch. I had lost not only CGM, but also my OpenAPS Artificial Pancreas that has been managing my glucose levels for six months.
I wrote about having a Treatment Continuity Plan here, but not for one moment did I think that I was going to have to enact it! But I have, and it made me think about the above points, but also the disaster case.
I have had to go back to SMBG to manage levels. I’m not doing it according to DAfNE, but more according to Sugar Surfing principles. I’m testing every 1-2 hours just to ensure I have a tab on what’s going on, then half an hour before meals to determine what I’m doing for the coming meal, to set appropriate boluses on the pump. At least I have a pump I can use for complex bolusing. But it’s mostly manual maths and manual decisions, unlike the use of Advanced Meal Assist on OpenAPS, where I’ve basically automated eating soon around my meal time, then bolused a bit before and then forgotten about it as it’s managed for me.
It’s a stark jump back in time. And a realisation of how lucky I am to be using such an amazing system. But to survive, we need to know how to do this stuff. We’ll continue to need to know. Technology can fail, and without knowing what to do in its place, you are setting up for disaster. It’s also helpful to have a basic understanding of what the technology is really up to. Just so you can spot if anything isn’t quite right. Technology is, after all, not 100% error free, although it’s close, and poor information in can easily result in an error coming out.
So what?
Realistically, if we really want to see more than 50% of T1Ds achieve the NICE targets, the model we use probably needs to change. But to do that comes at a significant cost. It requires tools that are currently not available to all, and in the future, are likely to be expensive.
Given the NHS principles in 1948 that good healthcare should be available to all, regardless of wealth, and the three core principles on which it was based:
- that it meet the needs of everyone
- that it be free at the point of delivery
- that it be based on clinical need, not ability to pay
Should we be able to offer today’s and tomorrow’s technologies to all T1Ds? Is it a clinical need to have the best possible chance of living with minimum complications, or is it simply a clinical need to be able to stay alive and live a reasonable standard of life? What is a reasonable standard of life, and who gets to make that decision?
That’s as much an ethical and political decision as it is a healthcare one. And it sits at the core of all the available technologies that we now have.
How much is one, pain and complication free, life really worth?

This is fascinating
I am a 56yr old T1D ( picking up the acronyms fast ) this blog is an eye opener but feel I have jumped in a) at the deep end, b) in the middle of the ocean. Please can you direct me to a good and easy starting point. I am MDI and had a half day DAFNe training about 20 years ago, so yes I struggle to get anywhere near 6% . When I really really try , cut down all carbs and finger prick and adjust 10+ times a day then I can get close, but never lower than 8.5% / 7.9% and I thought that was the way of all T1’s… that is till I happened on your blog, after googling T1D male actuarial life expectancy of all things as I look for pension annuities ( not very encouraging reading BTW) ! So to discover there is a better way/ alternative way of living with insulin has sparked a desire to learn more.
My GP is busy , so therefore next to useless, with a ‘wait and see’ answer to most things , and I have no diabetic specialist consultant or ‘team’ from whom to seek second opinion…. What should I be asking for / expecting of my GP ? I’d appreciate if you could point me to a ‘newbie ‘ T1 resource so I can do some study before I reapproach my GP! I am on glargene long acting and Humalog on MDI .many thanks once again for such an eye opening and insightful blog …howie
Hi Howie, thanks for stopping by. I’m glad that I’ve been able to help! I don’t know where in the country you are, but firstly, with your GP, ask that they refer you to a Diabetes specialist clinic. You should have had this for some time, and if you are interested in some of the more technological treatments, http://www.inputdiabetes.org.uk are a UK charity that can help you gain access to technology like insulin pumps.
If you want to refresh your dose adjustment skills, http://www.bertieonline.org.uk is an online course that can help. There is also http://www.t1resources.uk, a curated collection of resources that may be of some use.
Finally, there are a number of social media that can be of assistance. On twitter search for #gbdoc for GB Diabetes Online Community twitter chats and the regular Wednesday evening tweet chat. Facebook has a number of groups that may help you, and the diabetes.co.uk/forum T1 forum has people with a wide variety of experience who are supportive of looking at things in different ways.
If you’d like to chat more privately, you can use the comment form in the disclosure section.
And of course you’re always welcome to comment back on here. I hope that helps and do let me know how you get on.