Published today, the National Diabetes Audit reports from 2013-2015 are here and have some interesting findings for us. Participation in the audit by Clinical Commissioning Groups (CCGs) and Local Health Boards (LHBs) compared to previous years was down by a third, but from a T1 perspective we can see clear improvements in long term blood glucose levels and access to structured education. A high portion of T1s still struggling with managing blood glucose levels, a low participation rate in structured education and both significant variability of T1 care by CCG and LBH and a reduction in completion of critical care processes indicate areas where improvements are still needed.
But on to the data…
Treatment Targets
Cholesterol levels have remained constant, and with the ongoing questions that are now being raised as to the validity of Cholesterol research on which targets were based, I question whether this should be ignored. What’s interesting about the table (taken from one of the published presentations rather than the base statistics) is that the NICE Hba1C target is omitted.
Structured Education
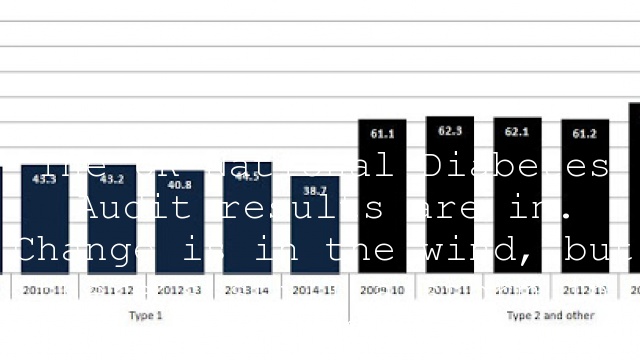
The number of people being offered education has dramatically increased over the past two years of the study, with nearly 76% of all diabetics in England and Wales being made this offer. The graph below shows how dramatic that change is.
Whilst showing a fundamental shift in thinking about the importance of structured education in diabetes care, what this graph hides is the disparity of availability of structured education for T1s and T2s.
It was offered to 78% of T2s but only 32% of T1s. What the reports don’t show, and what you need to dig down into the data for is the change in T1s.
- In 2012-2013, only 3.7% of all newly diagnosed T1s were offered structured education.
- In 2013-2015, 30% and then 32% respectively of newly diagnosed T1s were offered structured education.
The improvement is dramatic and welcome. And absolutely necessary. Now to get those long term T1s that still need education into some.
What’s perhaps more disappointing is the actual participation in Structured Education. In 2012-2013, 23% of those offered took it up. In 2014-2015, only 5.7% took it up. So while there was ten times more on offer, only three times as many people took it up. I think this highlights that delivery of the education on offer perhaps needs re-evaluating so that more participate.
Primary Care Processes

More disturbingly, as a T1 the variation between CCGs on the completion of primary care processes is fairly wide when compared with that seen for T2s. Again, this may not be solely down to the CCGs and LHBs, but may be much more a reflection of the age and socio-economic status of those diagnosed with T1 compared to T2. We already know that those under 40 have fewer completions, so laying the numbers of under 40s across the reporting CCGs, and adding the socio-economic status of the area may provide some interesting insights.
What is certainly true is that the GP-centred model feeding into mothership hospitals isn’t working and needs to be changed. These metrics aren’t good enough to stop a lot of people ending up in a place that the NHS just doesn’t want and we simply can’t continue in this vain.
Conclusions
It’s clear that it isn’t those in the top 30% that need help, rather those in the bottom 70%. The big question is how can this be achieved?




Leave a Reply